
In today’s intense healthcare environment, partnerships between acute and post-acute providers have been particularly essential. Though all post-acute settings provide value to their most appropriate patient types, they are not all created equal.1
Long-term acute care hospitals (LTACHs) have specific strengths that make them important partners for traditional hospitals. This has become particularly evident during the pandemic, as reported in a new study, Role of LTAC Hospitals in COVID-19 Pandemic, conducted by ATI Advisory using claims data from the Centers for Medicare and Medicaid Services (CMS). Supporting this conclusion, one Medical Director in a California-based physician group stated in the study, “LTAC hospitals can deliver a breadth of services and continuum of care for steady state acute patients in a way that decompresses the overburdened acute care system.” 2
This guide outlines three key advantages of LTACHs among post-acute partners that emerged in ATI research conducted during the pandemic.
LTACHs provide the most appropriate level of care for increasingly medically complex patients
Recent data have shown that patients have been admitting to short-term acute care hospitals (STACHs) with increasingly complicated conditions, magnifying the need to properly identify an appropriate recovery path. One VP of population health management highlighted this challenge, observing, “Most patients we discharge are still too complex for SNFs and they stay in the hospita.”3 However, delays in discharge can limit available capacity for new patients requiring stabilization in an STACH, a concern that came to the forefront during the pandemic.
LTACHs, with their ability to provide ICU-level treatment, have proven to be the most appropriate next level of care for medically complex patients, both before and during the COVID-19 crisis. The ATI research concluded that “initial claims data analysis from the beginning of the pandemic suggests that LTAC hospitals have remained a specialty setting appropriate for specific patients” as demonstrated by changes in Case Mix Index (CMI) and average length of stay (ALOS) according to CMS data.4
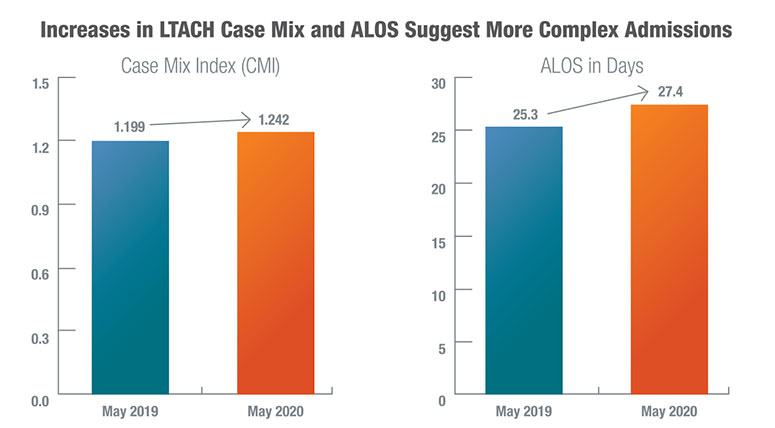 Source: ATI Advisory analysis of 100% Medicare FFS National claims incurred May 2019 and May 2020 and paid through June 2020. Note: Changes are more significant on a regional basis.
Source: ATI Advisory analysis of 100% Medicare FFS National claims incurred May 2019 and May 2020 and paid through June 2020. Note: Changes are more significant on a regional basis.
From May 2019 to May 2020, the CMI and ALOS at LTACHs increased by 3.6% and 8.3% respectively.5 Throughout this time, LTACHs clearly demonstrated their specific advantage among post-acute care providers in treating this unique patient population. According to the ATI study, under pandemic conditions, SNFs were twice as likely as LTACHs to readmit a patient to an STACH. Further, this divergence in outcomes had existed throughout the previous year, suggesting the relative advantage of LTACHs, while intensified during the pandemic, is not exclusively related to COVID-19.
Throughout the research, LTACHs proved to be the most appropriate level of care for patients who still require ICU-level treatment, but need to move from an STACH for capacity considerations.
Infectious disease protocols at LTACHs strengthen COVID, and future epidemic, containment
LTACHs also excel in treating and controlling infectious diseases, a skill that became particularly essential during the public health crisis. LTACHs are equipped with on-site laboratories, dialysis and negative pressure isolation rooms that allow them to minimize outpatient service needs and therefore reduce the risk of spread. Patients also benefit from interdisciplinary clinician teams with infectious disease specialists. Additionally, infection control standards, overseen by an Infection Prevention Nurse, comply with the requirements of CMS for general acute care hospital licensing.
These protocols are unmatched by most other post-acute care providers. While lower levels of care, such as SNFs, that have admitted COVID patients have faced challenges in preventing spread of the disease to their non-COVID residents, LTACHs largely contained further infection.6
According to ATI research, “The ability to cohort and separate care for non-COVID and COVID-positive patients has been a critical tool for STACHs, and a key contribution of LTAC hospitals during the pandemic. In certain markets LTAC hospitals continue to be the only facilities admitting COVID-positive patients, due to specialized COVID-19 units and the ability to safely separate patients.”7
Infection control will continue to be of utmost importance throughout the pandemic, and during future seasonal epidemics. With the goal of discharging patients to home as quickly as is safe, it will be important for providers to monitor the infection control protocols of downstream partners.
LTACHs provide pulmonary expertise essential in treating growing instances of respiratory conditions
A third benefit of LTACHs that has recently been highlighted is their expertise in caring for patients with pulmonary conditions such as pneumonia and acute respiratory distress, which is critical in the treatment of and recovery from COVID-19. Instances of acute respiratory distress syndrome and acute respiratory failure have continued to afflict the American population over the past five years. Research has shown that the pandemic and the seasonal flu can compound the severity of the existing pulmonary concerns, leading to surges in respiratory needs.8
As traditional hospitals face increased demand for pulmonary care, they are turning to LTACHs to assist in treating these patients. According to a pulmonology hospitalist specialist interviewed by ATI, “LTAC hospitals differentiate themselves because they have a laser focus on patients who are ventilator dependent, have respiratory failure, require dialysis, and have complex [post] surgical needs, etc. – all of that requires a multidisciplinary approach [in which] LTAC hospitals specialize.”9
At an LTACH, respiratory patients receive daily physician oversight, including care from a team led by pulmonologists, and benefit from respiratory therapy. These clinicians are highly specialized in their ability to liberate ventilator-dependent patients and understand the importance of incorporating mobilization as early as is safe and possible into the recovery plan for patients.
This expertise has not only been growing in importance as respiratory disease becomes increasingly prevalent but was also especially critical in the treatment of COVID and post-COVID patients.
Kindred Long-Term Acute Care Hospitals: An Experienced STACH Partner
The Kindred Difference
For more than 30 years, Kindred Hospitals have been the partner of choice for many health systems around the country. With daily physician oversight, ICU/CCUlevel staffing and specially trained caregivers, Kindred Hospitals work to improve outcomes, reduce disruptive and costly readmissions and help patients transition to a lower level of care. They are also committed to pursuing innovations in care delivery and payment models. One such initiative is the pursuit of disease-specific certifications, including in Respiratory Failure, from The Joint Commission in all Kindred Hospitals across the country in order to provide patients with an even higher level of clinical expertise.
Partnering Against a Pandemic
The pandemic of 2020 highlighted Kindred’s ability to be a flexible, acute-care partner. Kindred’s LTACHs played a critical role in public health efforts by closely aligning with STACHs across the country to relieve capacity constraints and deliver necessary hospital-level services to a more clinically complex population, including non-COVID and COVID patients.
One example of this partnership was in Houston, where Kindred Healthcare aligned with with a major STACH health system to provide additional capacity and resources to care for the surge of patients coming into the ICU. The system’s CEO noted the benefit of such close partnership: “We’re very appreciative that the barriers that typically exist in normal times have been taken out of play, and that’s helped us tremendously.”10 These hospitals, as well as others throughout the nation, worked in lockstep to form a united front against the pandemic.
Because of Kindred’s commitment to infection control and their skill in treating complex patients and pulmonary conditions, from 2019 to 2020, despite the pandemic, Kindred increased the percentage of Medicare fee-for-service compliant patients discharged to home by more than 6% year over year, and decreased the percentage discharged to an STACH to just over 8%, a more than 10% decrease from the previous year.11
The public health emergency created an intense healthcare environment from which Kindred and their STACH partners gained knowledge in dealing with surges in acute-care needs. Building on decades of experience, Kindred Hospitals will continue to be a valuable STACH partner in helping complex and critically ill patients reach their fullest potential for health and healing.
If you have a post-COVID patient, or other patients in need of continued acute care, call a Kindred Clinical Liaison for a patient assessment. Our experts will help you determine whether an LTACH stay is appropriate for your patient. If you are unsure of who your Kindred representative is, please feel free to contact us via recoveratkindred.com and speak with a Registered Nurse who can assist.
References
1-7: https://atiadvisory.com/wp-content/uploads/2021/02/Role-of-LTAC-Hospitals-in-COVID-19-Pandemic.pdf
8: https://journal.chestnet.org/article/S0012-3692(20)34937-0/fulltext
9: https://atiadvisory.com/wp-content/uploads/2021/02/Role-of-LTAC-Hospitals-in-COVID-19-Pandemic.pdf
10: https://www.aha.org/system/files/media/file/2020/08/aha-cs-kindred-health-0820%20%28006%29.pdf
11: Kindred internal data
April 19, 2021
[ad_2]
